Translate this page into:
Diagnosing breast hamartomas: Key radiological findings and differential diagnoses
*Corresponding author: Prama Dubey, Department of Radiodiagnosis, Sawai Man Singh Medical College and Hospitals, Jaipur, India. dubeyprama@gmail.com
-
Received: ,
Accepted: ,
How to cite this article: Dubey P, Modi PG, Sharma S, Bagarhatta M, Mannan N. Diagnosing breast hamartomas: Key radiological findings and differential diagnoses. Indian J Breast Imaging. doi: 10.25259/IJBI_26_2024
Abstract
Fibroadenolipomas, or hamartomas are rare, benign masses can occur in the breast. They are often asymptomatic but can present as soft, mobile lumps. The masses can be diagnosed with their typical mammographic, sonographic and magnetic resonance imaging (MRI) findings due to their diverse tissue components. We report the typical imaging features of a breast hamartoma on ultrasonography and MRI in a young female. Given the benign nature of the lesion, no surgical intervention is required unless there is significant symptomatology or a change in the clinical presentation.
Keywords
Fibroadenolipoma
MRI breast
USG breast
INTRODUCTION
Breast hamartomas, also referred to as fibroadenolipomas, are benign breast masses that occur due to the proliferation of fibrous, glandular, and fatty components—hence the name fibroadenolipoma.[1] These typically occur in women over 35 years of age and may be discovered incidentally in an asymptomatic female during mammographic screening. They can also present as soft, mobile, non-tender breast lumps. The typical appearances of these masses on various imaging modalities help diagnose the lesions. Despite their benign nature, distinguishing breast hamartomas from other neoplastic lesions is crucial for appropriate management. This case report highlights the clinical, radiologic, and histopathologic features of a breast hamartoma, with an emphasis on the importance of imaging techniques in making an accurate diagnosis and differentiating it from other potential breast pathologies.
CASE REPORT
A 17-year-old female patient presented to us with a complaint of a palpable lump in the left breast for the past 6 months, located in the upper outer quadrant. On examination, the lump was soft, mobile, and non-tender. The patient reported no history of trauma, pain, or nipple discharge. There were no skin changes. There was no family history of breast cancer. She had no children.
Imaging Findings
High-resolution ultrasound of the left breast was performed using a linear probe. A well-circumscribed, heterogeneous mass was seen in the upper outer quadrant of the left breast [Figure 1]. The mass had smooth, well-defined margins and did not show significant internal vascularity on color Doppler imaging. There was no posterior acoustic shadowing or intralesional calcifications. Surrounding breast tissue appeared normal. No axillary lymphadenopathy was seen. Based on the ultrasound findings, a provisional diagnosis of breast hamartoma was suggested, and a breast imaging reporting and data system (BIRADS) 2 category was assigned to it.
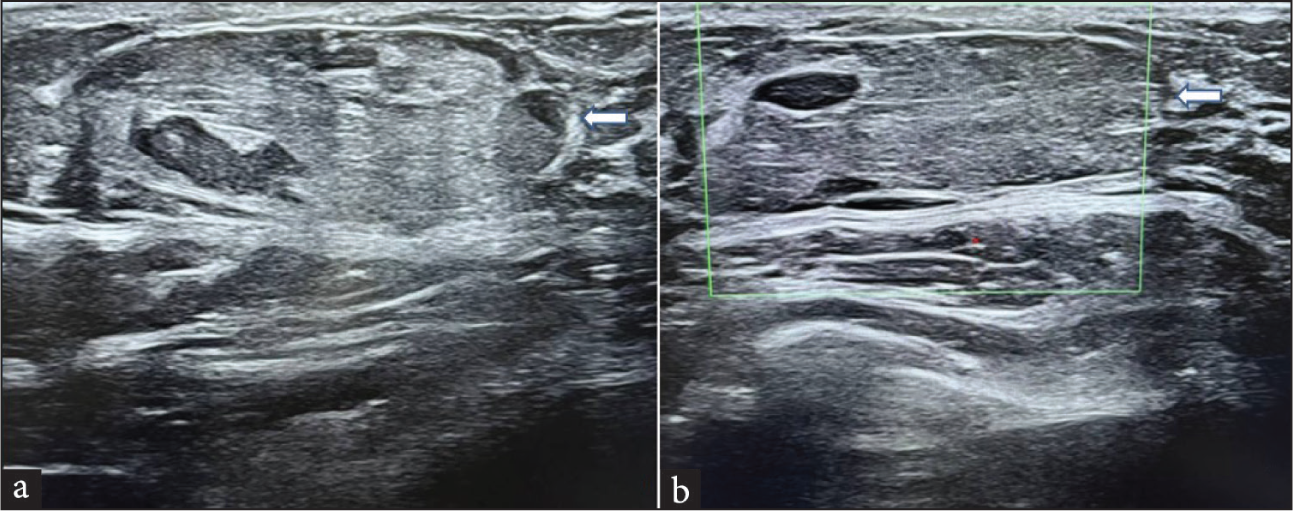
- Ultrasound of the breast demonstrated (a) a well-defined heterogeneous mass with central fatty and surrounding hypoechoic echopattern (white arrow). There was no posterior acoustic shadowing or enhancement. (b) On color doppler imaging, the mass did not show any appreciable internal vascularity (white arrow).
Dynamic contrast-enhanced magnetic resonance imaging (MRI) of both breasts was performed for confirmation of diagnosis and for ruling out a malignant mass or malignant transformation. A well-circumscribed mass was seen in the upper outer quadrant of the left breast, showing mixed signal on both T1-weighted and T2-weighted sequences with areas of fat showing suppression on short tau inversion recovery (STIR) sequences [Figure 2]. No diffusion restriction was noted. The mass demonstrated progressive and persistent peripheral nodular enhancement and a type 1 curve on the kinetic graph. No associated skin thickening or suspicious lymphadenopathy was seen.
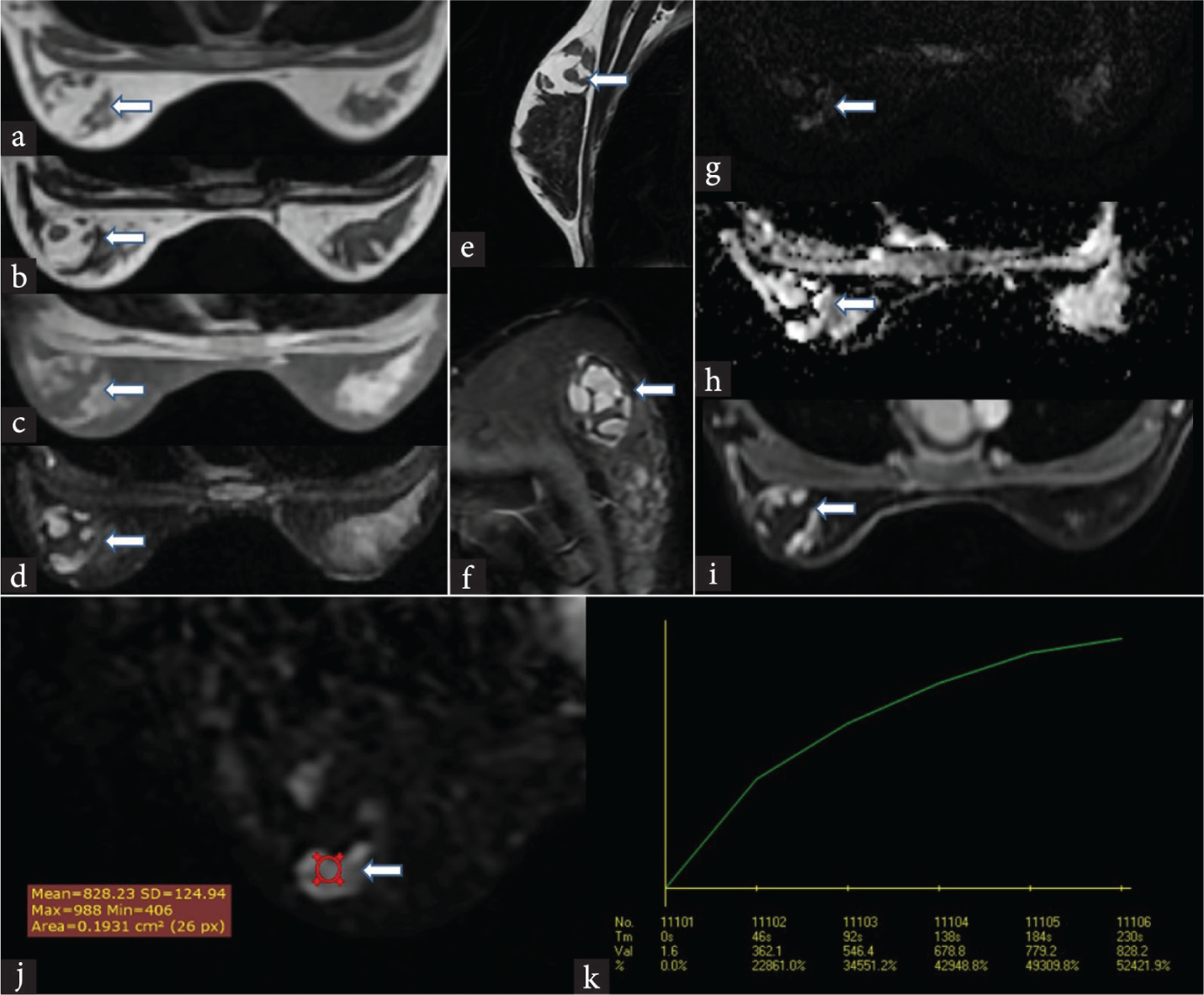
- MRI breast showed a (a) T1 and (b) T2 heterogeneous mass in the upper outer quadrant of the left breast (white arrows). The mass showed central area fat suppression on (c) T1 and (d) T2 fat-suppressed imaging (white arrows). (e) Sagittal T2-weighted images of the mass show a smooth, thin peripheral capsule (white arrow). (f) Coronal STIR images confirm the central fat within the lesion (white arrow). The breast mass did not show any diffusion restriction on (g) diffusion-weighted images and (h) apparent diffusion coefficient (ADC) map (white arrows). (i) There was peripheral, nodular enhancement on contrast-enhanced imaging (white arrow). (j) A time-intensity curve was obtained for the enhancing part of the mass (white arrow). (k) A type 1 curve was obtained. The grey box indicates the region of interest (ROI)- the breast tissue at which the time intensity curve was obtained. STIR: Short tau inversion recovery.
Based on the ultrasonography (USG) and MRI findings, a diagnosis of breast hamartoma was suggested and was assigned a BIRADS 2 category. The patient was reassured, and routine self-breast examinations and clinical follow-up were advised. She was asked to return for a clinical and radiological follow-up if she noticed any changes in size, shape, or palpability of the mass.
DISCUSSION
Breast hamartomas are benign lesions composed of an abnormal mixture of glandular tissue, fibrous tissue, and fat.[1] Although rare, they can occur at any age, typically presenting in women between 15 and 35 years. The patient in this case report was a 17-year-old female. Hamartomas are often asymptomatic, but when symptomatic, they present as painless, mobile, palpable masses, as seen in this case, wherein the patient noticed a painless, soft breast lump.
On mammograms, a hamartoma is seen as a well-circumscribed, round, or oval mass surrounded by a thin capsule. The fat component within the hamartoma appears radiolucent, and the soft tissue component appears radiodense. The classical appearance of a “breast within a breast” is described.
On ultrasound, breast hamartomas typically appear as well-circumscribed, solid masses with smooth margins, which is consistent with the findings in this case. They may have heterogeneous echotexture. The lack of internal vascularity on Doppler imaging further supports the benign nature of the lesion. The absence of posterior acoustic shadowing helps differentiate hamartomas from other solid breast masses, such as fibroadenomas, which can sometimes cause shadowing.[1]
Hamartomas are typically benign but may rarely present with breast malignancy, which can develop in the glandular component of the mass. A contrast-enhanced MRI of the breasts can help identify a malignant focus within a hamartoma, in addition to confirming the diagnosis.[2] MRI findings of hamartomas typically demonstrate a well-defined mass which exhibits heterogeneous signal intensity on T1 and T2 sequences due to the presence of glandular and adipose tissue components and a thin capsule.[1] After administration of contrast medium, hamartomas show a gradual, progressive enhancement of the fibroglandular elements with a type I time/intensity curve.[3] If suspicious features are noted, especially on mammography or ultrasound, contrast-enhanced MRI can be useful in establishing a diagnosis. The hamartomas do not show aggressive features such as irregular borders, spiculations, or axillary lymphadenopathy, all of which are concerning for malignancy.
There is a limited role of fine needle aspiration cytology and needle core biopsy in diagnosing a breast hamartoma. Clinical examination and radiological investigations help to avoid underdiagnosis of these masses.[4] However, atypical appearances of breast hamartomas necessitate histopathological examination to rule out malignancy. These appearances include dense masses on mammograms with benign-appearing calcifications and hyperechoic or hypoechoic lesions on ultrasounds with complete or incomplete posterior shadowing.[5]
Recommendations: Routine clinical follow-up as the lesion is benign. No immediate intervention is required unless there is a change in the mass characteristics or symptoms. If the patient becomes symptomatic or if the lesion increases in size, further evaluation may be warranted.
DIFFERENTIAL DIAGNOSES
Fibroadenoma: A common benign breast tumor composed of fibrous and glandular tissue. Fibroadenomas usually present as well-defined, hypoechoic masses on ultrasound. However, fibroadenomas may show posterior acoustic shadowing, which is not observed in hamartomas.
Breast lipoma: A benign lesion composed of mature adipose tissue. Lipomas are typically well-defined, homogeneously hyperechoic masses on ultrasound and demonstrate a uniform fatty appearance on MRI. The patient’s lesion, which is heterogeneous and shows mixed tissue characteristics, is more consistent with a hamartoma than a lipoma.
Phyllodes tumor: A rare fibroepithelial tumor that may present as a rapidly growing breast mass. On imaging, phyllodes tumors may show well-defined borders, but they can also demonstrate cystic degeneration, irregular edges, and rapid growth.
CONCLUSION
The imaging findings of the well-circumscribed, heterogeneous, non-vascular mass on color Doppler with internal fatty areas and type 1 enhancement on MRI suggest the diagnosis of a breast hamartoma. A typical breast hamartoma demonstrates no characteristics concerning malignancy, and the clinical course is expected to be benign. Although diagnosis may be made on a combination of mammography and ultrasound, dynamic contrast enhanced MRI should be performed to look for any underlying malignant change. Further follow-up may not be necessary in a benign hamartoma if the mass remains stable, but clinical monitoring should be considered to ensure no changes in size or character over time.
Ethical approval
Institutional Review Board approval is not required.
Declaration of patient consent
The authors certify that they have obtained all appropriate patient consent.
Financial support and sponsorship
Nil.
Conflicts of interest
There are no conflicts of interest.
Use of artificial intelligence (AI)-assisted technology for manuscript preparation
The authors confirm that there was no use of artificial intelligence (AI)-assisted technology for assisting in the writing or editing of the manuscript and no images were manipulated using AI.
REFERENCES
- Breast hamartoma: Ultrasound, elastosonographic, and mammographic features. Mini pictorial essay. J Ultrasound. 2015;18:373-7. [Last accessed on November 28 2024]. https://doi.org/10.1007/s40477-015-0175-0
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Invasive ductal carcinoma arising within a large mammary hamartoma. Breast J. 2015;21:196-7. [Last accessed on November 28 2024]. https://doi.org/10.1111/tbj.12378
- [CrossRef] [PubMed] [Google Scholar]
- “Breast within a breast” sign: Mammary hamartoma. Med J Armed Forces India. 2015;71:377-9. [Last accessed on November 28 2024]. https://doi.org/10.1016/j.mjafi.2015.06.009
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Hamartoma of the breast: A clinicopathological review. J Clin Pathol. 2002;55:951-4. [Last accessed on November 28 2024]. https://doi.org/10.1136/jcp.55.12.951
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]
- Invasive ductal carcinoma in a mammary hamartoma: Case report and review of the literature. Korean J Radiol. 2010;11:687-91. [Last accessed on November 28 2024]. https://doi.org/10.3348/kjr.2010.11.6.687
- [CrossRef] [PubMed] [PubMed Central] [Google Scholar]








